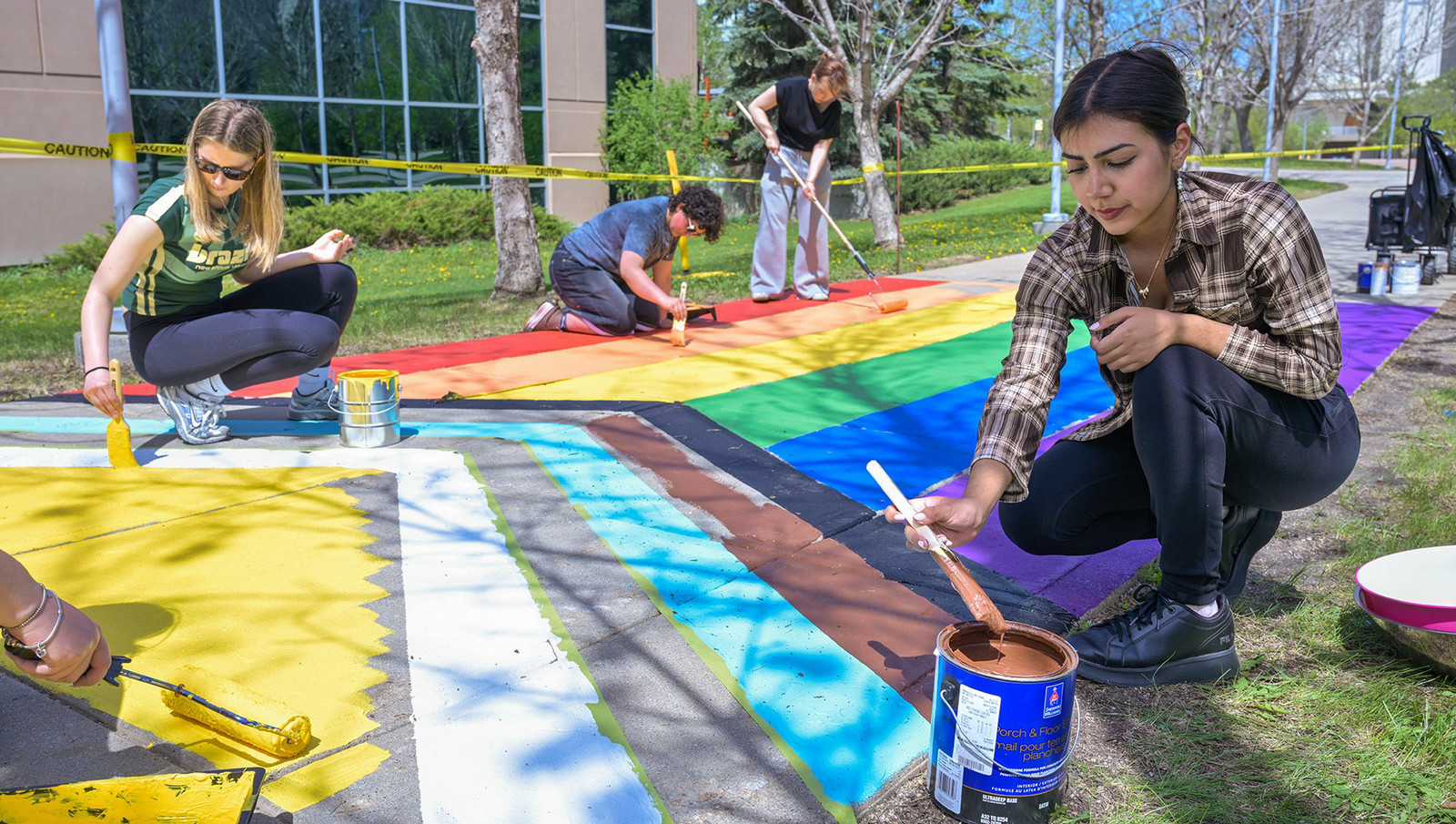U of R Stories

Lock and Loan: How Archer Library & Archives is Making Cycling More Accessible

Educating the Next Generation of Digital Marketers and Strategists
Recent Posts
Pride Month Adds a Splash of Colour to the U of R
The campus community came together to paint U of R sidewalks for Pride Month.
Lock and Loan: How Archer Library & Archives is Making Cycling More Accessible
The Dr. John Archer Library & Archives is making cycling to campus better for students, faculty and staff. The University’s Ride Ready...
Educating the Next Generation of Digital Marketers and Strategists
New Digital Marketing programs bridge the gap between high-level strategy and hands-on technical skills.
U of R Students Take the Stage at MusicFest Canada
Three U of R students represented Saskatchewan at MusicFest Canada, showing how music can shape futures on and off the stage.
Project Day 2026: U of R Engineering Students Showcase a Bright Future for Saskatchewan
At Project Day 2026, U of R engineering students unveiled capstone projects tackling carbon capture, agri-tech, soil remediation, and more for...
U of R Opens Innovative Nursing Virtual Reality Lab
The Faculty of Nursing’s new Virtual Reality Lab is preparing nursing students for the realities of clinical practice.
Best and brightest: U of R welcomes 14 future leaders on full Chancellor’s Scholarships
High-achieving, talented students from across SK and BC begin their studies at U of R this fall as recipients of the prestigious Chancellor’s...
New Video Celebrates Vision of University of Regina’s New Strategic Plan
Together, We Serve, the U of R’s new strategic plan video, captures the spirit, energy, and collective commitment driving the University...
Like Father, Like Son: A Journalism Legacy in the Classroom
Father-and-son duo Darrell and Austin Davis blend decades of experience with fresh digital perspectives as a teaching team for an advanced news...
AI Disinformation, Deepfakes, and the Fight to Protect What Is Real
From deepfakes targeting children to disinformation targeting Canada, Part 2 of the AI Futures series explores the AI-related threats impacting the...